In Rwanda, particularly in the
rural areas, children who die
from mysterious circumstances
are sometimes believed to have
been poisoned or bewitched.
Mulindo is a rural suburb of Kigali, the small but mighty capital of Rwanda. High in the hills, the suburb is a safe haven from the occasional mudslides during the rainy season and provides a glorious view of East Africa’s magnificent scenery. On many mornings, clouds float toward each other in the sky, promising rainy days. In the distance, birds chirp in the trees, perhaps announcing the coming rain or responding to the pigs oinking in a nearby pigsty.
But amidst the geographic beauty are many people who struggle to survive. Economic and social resource structures were deeply impacted by Rwanda’s 100-day genocide in 1994. The brutal genocide against the Tutsi people resulted in the loss of an estimated 500,000 to one million lives. While the many valleys offered refuge from the killings for some, they became graveyards for others. Many of those persecuted could neither withstand the long treks to refugee camps nor the long wait for rescue.

Three decades later, there are some positive signs of recovery. The country has seen strong economic growth, has one of the most robust healthcare systems in Africa, and is said to lead the continent in gender equality. However, more support is needed to ensure all residents of Rwanda have equitable access to resources, which can be exceptionally difficult for those who live in more rural areas.Particularly in the suburb of Mulindo—like in much of the world—there is a large gap between the poor and the rich. A housekeeper or security guard can earn as little as the equivalent of $15 USD a month and even a primary school teacher may only take home $50 USD a month depending on qualifications and experience.
Many of the suburb’s 30,000 residents live well below the poverty line and sacrifice greatly—leaving their homes and walking many miles to find work, relying on strenuous small-scale farming or struggling to find employment in the city center—to meet their families’ needs.
Shopping at the market or going to a health clinic or school requires costly bus trips or long walks through the hills. Those who are able to procure employment on small-scale farms are reliant on crop yields; the average pay for a day’s work is $1 USD when yields are good, which is intermittent. Those formally employed face similar struggles.
Meet Ineza and Rebeka
Rwandan Sisters
Living With Type 1 Diabetes


Sisters Ineza and Rebeka encapsulate Rwandan resilience. They were both diagnosed with type 1 diabetes—Ineza at 14 and Rebeka at 12.
Now at 14 years of age, Rebeka is very small in stature. Ineza, now 18, is even smaller than her younger sister and lacks the height and weight of her peers. Although their beautiful smiles eclipse their startlingly petite frames, their low growth rate and low body mass index hint at an underlying nutritional deficit, both from lack of food and years of inadequate diabetes care due to lack of access to vital medications and supplies.
Like the country in which they live, diabetes is a disease of countless hills and valleys—all those who live with the disease endure daily low and high blood sugar swings that impact energy, health and safety.
Type 1 diabetes is a chronic autoimmune condition that makes the body unable to produce insulin, a hormone that regulates blood sugar. Without insulin, people’s bodies cannot use the sugar in their bloodstream as energy, causing diabetic ketoacidosis (DKA), which can lead to a diabetic coma or even death. Nothing can be done to prevent or cure the disease.
Type 1 diabetes management is challenging and requires access to medical care, supplies and support. The best health outcomes are aided by consistent access to health care professionals trained in diabetes, as well as affordable access to insulin and blood sugar monitoring devices, a privilege afforded to few across the globe.
For people like Ineza and Rebeka, managing the highs and lows is dependent on receiving basic supplies through local diabetes organizations that survive on donor support.

Ineza started experiencing symptoms of her undiagnosed type 1 diabetes in 2018 at the age of 14. She took frequent trips to the bathroom, had low energy and was often dizzy. Like much of the world’s population, Ineza’s family and friends only knew about type 2 diabetes, more often diagnosed in adults and with a less severe onset. Because of this, they did not know what to make of Ineza’s ongoing symptoms.
By the time Ineza was diagnosed, her body was likely already undergoing the stages of the onset of type 1 diabetes for months. Without enough insulin in her system to process food and sugars into fuel, Ineza’s physical development slowed down. Additionally, a lack of proper nutrition led to stunted growth.
Because Rebeka was diagnosed second at age 12, the family recognized the symptoms of the disease and were able to get her a faster diagnosis and medical care. The illness has still affected her development too but an earlier diagnosis meant she fared better than Rebeka in her physical growth.
After diagnosis, Ineza was shunned by neighbors who assumed she had a contagious illness or HIV—an illness that still comes with a lot of stigma. Others believed that the children had been cursed by family enemies or jealous neighbors and thought they were under a curse or some sort of poisoning. In Rwanda, particularly in the rural areas, children who die from mysterious circumstances are sometimes believed to have been poisoned or bewitched.
Ineza and Rebeka are being raised by their single mother Francine Hakuzimana. Their family lives in two huts made from rukarakara, a type of mud that is fortified by straw into an almost brick-like stability. Next to the mud huts sits a pigsty containing two pigs and a goat. Plantain trees are scattered around the houses to provide the much-beloved staple food plantain, as well as shelter.

In addition to carrying the responsibilities of her home and six children—five of whom live with her, including Ineza and Rebeka—on her own, Francine is challenged by a stigma that many mothers in Rwanda face.
A saying in Kinyarwanda goes,
“ibigoryi ni ibya nyina”
“the mother is the one that
gives birth to abnormal children.”
The statement places blame on women
for giving birth to unhealthy children.
Because of this, Francine and her daughters were all shunned. At a time when they needed assistance the most, the girls and their mother found themselves at the edge of society with little to no financial and emotional support.
Francine is one of Mulindo’s small-scale farmers. She sells her seasonal harvest as well as manure to take care of those who depend on her. On days when Francine is unable to get the income she needs to buy food for the family, the girls will skip their essential insulin doses. Skipping insulin doses is dangerous. Although the girls receive diabetes care and education and—through efforts of local support organizations—now have access to the insulin they need to survive, limited resources still mean that what should be a manageable condition remains unpredictable and life-threatening for them.
Diabetes Care in Rwanda
An Uphill Battle
When both girls were diagnosed, they were referred by the local hospital to the Rwanda Diabetes Association (RDA), an institution that was founded in 1997 by the late François Gishoma. François himself had diabetes, so his founding of the RDA came from a deeply personal experience.
According to his son and chair of the RDA board of directors, Crispin Gishoma, François knew both the importance and the costs of frequent visits to the doctor as well as having meters and insulin at home to regulate blood sugar levels. He realized that unlike him, there were many who could not afford the life-sustaining medications and care. With this in mind, François founded the RDA in order to advocate for patients with diabetes in Rwanda.
Initially, the RDA faced great difficulty in even identifying patients with type 1 diabetes. Little was known about the disease and symptoms were often attributed to other causes. This has changed over time with health education efforts and growing access to health centers. The RDA, in partnership with global nonprofit Life for a Child, is now able to provide health care and resources to advocate for, treat and manage type 1 diabetes in 2,500 Rwandan people living with the condition.

Life for a Child is a nonprofit organization led by Graham Ogle, a pediatric endocrinologist. Life for a Child partners with diabetes centers in under-resourced countries to provide care for children and young people with diabetes. Graham shares that the organization was founded after the realization that young people with type 1 diabetes in contexts such as Mulindo’s faced extraordinary suffering in comparison to those in well-resourced countries.
“Many were dying very quickly because of lack of access to care and others were growing up with a poor quality of life, being chronically unwell and developing early and devastating diabetes complications because they couldn’t get access to care,” Graham says.
Emma Klatman, global policy and advocacy manager at Life for a Child
When Graham began having conversations with the RDA’s François about the state of diabetes care in Rwanda, François initially felt discouraged about identifying patients without being able to provide them with support. François shared with Graham how much he loathed having to say to a patient “best wishes” and then leaving without providing them a solution. In 2005, Life for a Child was able to step in and start providing those solutions—supporting François and the RDA’s existing network by providing the resources needed to truly change health outcomes. François could finally become excited about identifying patients; he could help them and provide them with life-saving solutions.
There have been many lives saved by the RDA’s work in Rwanda, but it is likely that many more are still being lost. With only three endocrinologists in Rwanda, all of whom are based in Kigali, patients living outside the capital remain without access to consistent diabetes care. More support is needed to expand the RDA’s reach.

To address these kinds of circumstances, Life for a Child announced Vision 2030, a 10-year plan to improve care for young people like Ineza and Rebeka.
The plan aims to help RDA offer a wider range of diabetes management options, strengthen diabetes education programs and upskill local health workers. In addition, they are actively searching for young people living with diabetes and in need of support in rural and currently underserved areas. Individual donors help bring this vision to life.
Since their diagnosis, Ineza and Rebeka have received insulin and syringes from the RDA. When their family is in dire need of food, the RDA also provides them with food parcels. Recently, during the stay-at-home order and lockdowns imposed to contain the spread of COVID-19, their mother Francine struggled to get the essentials needed to support her family. Unable to leave home to work, she found herself without any fall back, but the RDA lent her family a hand.
“The association has paid me visits [and] brought me food, rice, posho [a thick maize porridge], beans and the children ate and felt good,” Francine says. “I didn’t meet any challenge, [since] they brought me medicine at home.” The RDA has also given the family a goat to provide them with much needed manure.

Treatment and relief aid are not the only focus of the RDA. They run other programs to educate and empower patients and their families. The RDA’s vocational training program targets patients with type 1 diabetes who had to drop out of school from being too sick. Once identified, these patients receive vocational training and are able to pursue interests and career opportunities.
The RDA also holds annual camps to train patients on how to better care for their health. According to clinical coordinator for the RDA and Life for a Child, Etienne Uwingabire, the RDA’s ultimate goal is to reach every patient with diabetes in the country. “For the next five years, the Rwanda Diabetes Association has planned that every diabetic patient, especially those with type 1 diabetes, will receive one week training on their disease in a camp so that we can bring them together and teach them how to take care of themselves, how to live and how to feel confident,” Etienne says.
Thanks to the help they have received from the RDA and Life for a Child, Ineza and Rebeka now know their condition is not insurmountable.
Early on in their diagnosis, treating diabetes felt like an uphill battle that they were not sure they would win.
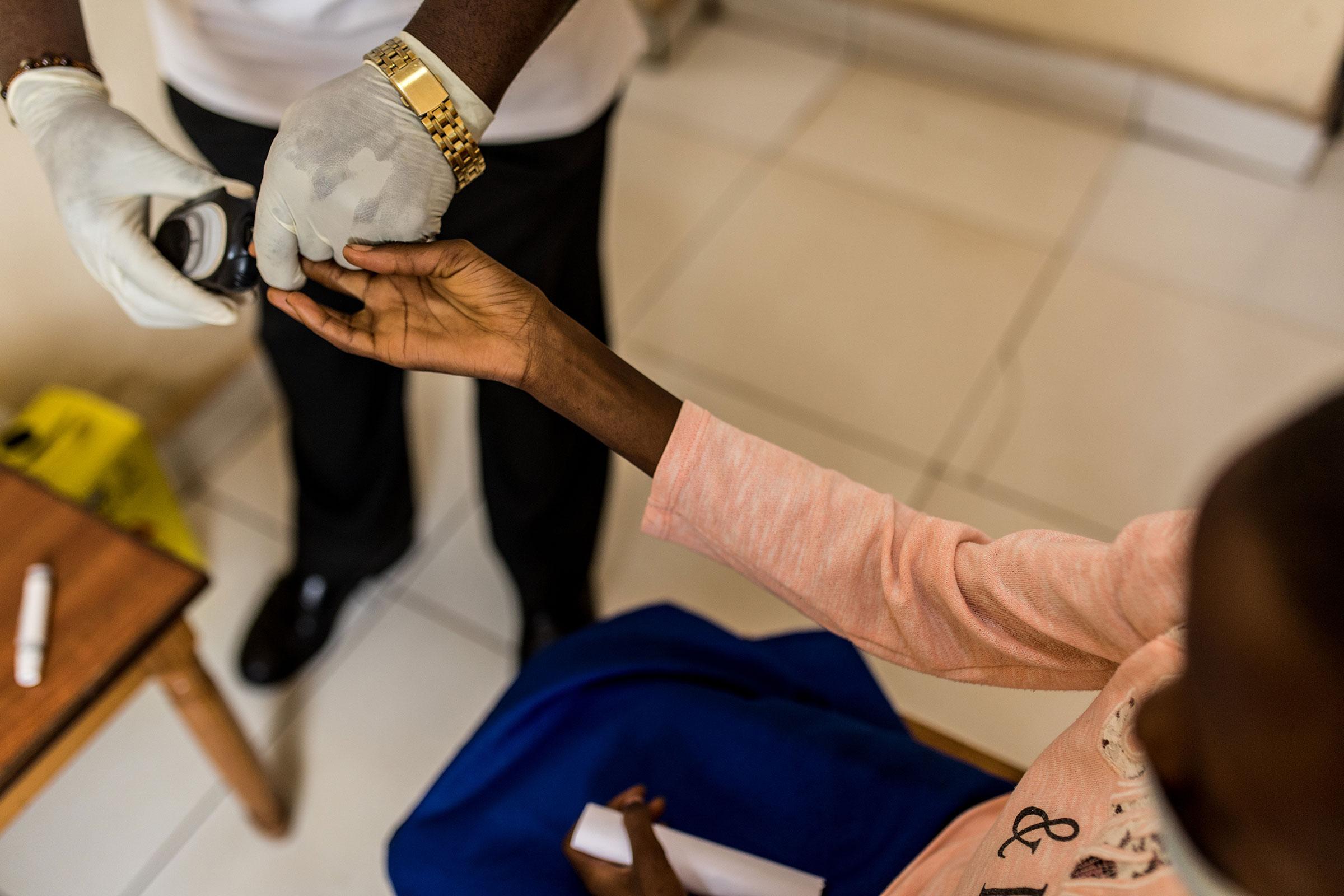
The RDA + Life for a Child:
Filling Gaps
in Mutuelle de Santé
To best understand the work of the RDA, it is important to first understand healthcare in Rwanda.
In 2005, the country launched a community-based health insurance program called Mutuelle de Santé. Reformed in 2011 to a tiered payment system, the plan is designed to give all Rwandan citizens access to healthcare regardless of their ability to pay—those who can afford to pay healthcare premiums do, while those who cannot afford it are still meant to be able to use Mutuelles by declaring their lower income to the government.
Those in the lowest income brackets are meant to receive care for free, but—as is often the case with health insurance plans across the globe—not everyone receives the access the system is designed for. It is estimated that at least 10% of Rwanda’s population is not covered.
In Francine’s case, constantly shifting financial circumstances based on the COVID-19 pandemic, events in her family and when she is able to access work have meant that she has not been able to declare her new, lower income and is currently still expected to pay for her family’s healthcare.
Her family’s annual contribution is the equivalent of $18 USD, a challenging amount to raise for someone with her meager resources and many responsibilities.

Francine is committed to paying for Mutuelles because she knows how much it benefits her daughters. But even once she finds the means to pay for healthcare, there are other costs attached to hospital visits or stays such as transportation, food and accommodation for an accompanying caregiver. At times, Francine is unable to meet these costs and has to make the difficult decision of caring for the girls at home. But more often than not, this results in further health decline for them, ultimately leading to hospital stays—and longer ones—being their only choice. There is a common Rwandan saying that translates universally: “if only a mother’s love could heal.”
She shares that when her son started showing symptoms, the hospital did not give him a diagnosis. “When he got sick, he had various symptoms and I went to the doctor at Muhima where we spent almost two weeks in critical condition. At that time, I remember that we didn’t get a diagnosis, so we decided to take him to another hospital,” she says.
Thankfully the second hospital probed further and ran more tests. Because of the delay in identifying his condition, he fell into a coma but fortunately was able to come out of it once he received medical care. The first hospital where they were not able to receive a diagnosis was public, so it was paid for by Mutuelles. The second hospital was private, therefore did not accept the public healthcare plan. Private care must be paid for with cash or private insurance, which costs upward of $150 USD per year depending on the plan.
“Sometimes we are sent to the health center, [but] the health center doesn’t have enough of these medications at the time, [so] they then transfer us to King Faisal Hospital which doesn’t work with Mutuelle de Santé,” Viviane shares. The RDA’s intervention has been a source of security in times like this.

Ineza and Rebeka visit the RDA at Kinamba, an hour’s bus ride from Mulindo, once a month to collect insulin and syringes. But, in the land of a thousand hills, a trip to the local bus stop is too strenuous and the girls must take a motorbike taxi to catch the bus. Altogether, Francine spends an estimated $15 USD to get the girls to the RDA and back, adding to the financial burden of the family.
“I don’t get any income and even when I get some, I spend it on food,” Francine says. “It is even a miracle when I get them transport money to go to the association once a month; I sometimes ask for lifts on the road and they sympathize with us, they give us a ride for free.”

More Support Will Change
the Lives
of People With
Diabetes in Rwanda
There is still a stigma associated with individuals who have diabetes in Rwanda. Many consider people with diabetes to be a burden and some even believe they brought the disease on themselves by consuming too much sugar. But this lack of knowledge about type 1 diabetes leads to lack of proper care, which impacts livelihood. Frequent absences from school and work result in underperformance, which frustrates both teachers and employers. It becomes a vicious circle.
As the RDA and Life for a Child’s Etienne shares, “serious problems we are facing include first convincing diabetics and their families that diabetes is not a problem but to get information about it. Another one of the major problems we face is that people don’t understand it very well; self-acceptance is very difficult, it takes effort to convince someone.”

For Ineza and Rebeka, getting access to information about diabetes from the RDA—in addition to access to insulin and medical support—has been vital. The girls share that since getting diagnosed, they have accepted living with type 1 diabetes. Neighbors are kinder and more accepting while classmates are helpful when the girls need assistance. Community members also have invited the family back into their homes.
Ineza and Rebeka are both in sixth grade. Their illness has held them back in a lot of ways, including missing many school days. This has resulted in repeated academic years. Despite this, they are excited about being in school and learning.
Ineza loves Kinyarwanda and mathematics while Rebeka enjoys social studies and English. Both girls have ambitious goals after their studies. “I want to become a doctor when I grow up,” Ineza says. “So that I can take care of other patients like doctors take care of me too.”
Help Life for a Child deliver
life-saving diabetes care globally.



CREDITS:
Interviews + Research: Laurien Sibomana, Crispin Gishoma
Writing: Henriette Mushimiyimana
Editing: Rachel Clayton, Lala Jackson, Sevde Kaldiroglu, Emma Klatman, Dr. Graham Ogle, Sumithira Thavapalan
Photography: Jacques Nkinzingabo
Videographer: Cedric Ishimwe
Video Editing: Isaac Nkinzingabo Rudakubana
Site Design: Beyond Type 1
Map design: DGFX and courtesy of: Cartifact
The names of some people and places have been changed to protect the identity of young people supported by Life for a Child.